Nasopharyngeal Cancer
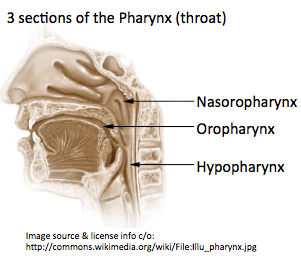 The nasopharynx is the upper part of the pharynx (throat) behind the nose. Nasopharyngeal cancer occurs when the cells of the nasopharynx become abnormal and start growing in an uncontrolled way. The majority of nasopharyngeal cancers are squamous cell carcinomas (squamous cells are the thin, flat cells in the lining of the nasopharynx), but there are a number of other different types.
The nasopharynx is the upper part of the pharynx (throat) behind the nose. Nasopharyngeal cancer occurs when the cells of the nasopharynx become abnormal and start growing in an uncontrolled way. The majority of nasopharyngeal cancers are squamous cell carcinomas (squamous cells are the thin, flat cells in the lining of the nasopharynx), but there are a number of other different types.
 Information for Patients and the Public
Information for Patients and the Public Information for Health Professionals / Researchers
Information for Health Professionals / Researchers Latest Research Publications
Latest Research PublicationsInformation Patients and the Public (7 links)
 Nasopharyngeal Cancer Treatment
Nasopharyngeal Cancer Treatment
National Cancer Institute![]() PDQ summaries are written and frequently updated by editorial boards of experts Further info.
PDQ summaries are written and frequently updated by editorial boards of experts Further info.
Cancer Research UK![]() CancerHelp information is examined by both expert and lay reviewers. Content is reviewed every 12 to 18 months. Further info.
CancerHelp information is examined by both expert and lay reviewers. Content is reviewed every 12 to 18 months. Further info.
Cancer.Net![]() Content is peer reviewed and Cancer.Net has an Editorial Board of experts and advocates. Content is reviewed annually or as needed. Further info.
Content is peer reviewed and Cancer.Net has an Editorial Board of experts and advocates. Content is reviewed annually or as needed. Further info.
 Nasopharyngeal cancer (cancer of the nasopharynx)
Nasopharyngeal cancer (cancer of the nasopharynx)
Macmillan Cancer Support![]() Content is developed by a team of information development nurses and content editors, and reviewed by health professionals. Further info.
Content is developed by a team of information development nurses and content editors, and reviewed by health professionals. Further info.
American Cancer Society
Throat Cancer Foundation
Summary and details of symptoms.
Mayo Clinic
Information for Health Professionals / Researchers (7 links)
- PubMed search for publications about Nasopharyngeal Cancer - Limit search to: [Reviews]
PubMed Central search for free-access publications about Nasopharyngeal Cancer
MeSH term: Nasopharyngeal Neoplasms US National Library of Medicine
US National Library of Medicine PubMed has over 22 million citations for biomedical literature from MEDLINE, life science journals, and online books. Constantly updated.
PubMed has over 22 million citations for biomedical literature from MEDLINE, life science journals, and online books. Constantly updated.
 Nasopharyngeal Cancer Treatment
Nasopharyngeal Cancer Treatment
National Cancer Institute![]() PDQ summaries are written and frequently updated by editorial boards of experts Further info.
PDQ summaries are written and frequently updated by editorial boards of experts Further info.
START, European School of Oncology
Detailed referenced article.
Medscape
Detailed referenced article by Arnold Paulino, MD.
Radiopaedia.org
Referenced article with radiology images by Radswiki and Dr Frank Gaillard.
Patient UK
Referenced article covering cancers of the oropharynx, hypopharynx, and nasopharynx.
The Enigmatic Epidemiology of Nasopharyngeal Carcinoma
Cancer Epidemiol Biomarkers Prev October 2006 15; 1765
Chang E, Adami HO (2006)
Latest Research Publications
This list of publications is regularly updated (Source: PubMed).
Self-assembled peptido-nanomicelles as an engineered formulation for synergy-enhanced combinational SDT, PDT and chemotherapy to nasopharyngeal carcinoma.
Chem Commun (Camb). 2019; 55(69):10226-10229 [PubMed] Related Publications
SOX9 promotes nasopharyngeal carcinoma cell proliferation, migration and invasion through BMP2 and mTOR signaling.
Gene. 2019; 715:144017 [PubMed] Related Publications
Interferon beta increases NK cell cytotoxicity against tumor cells in patients with nasopharyngeal carcinoma via tumor necrosis factor apoptosis-inducing ligand.
Cancer Immunol Immunother. 2019; 68(8):1317-1329 [PubMed] Related Publications
PATIENTS AND METHODS: NK cells and serum samples from two patients with NPC were analyzed before and at different time points during IFNβ therapy, for assessment of TRAIL expression and NK cell cytotoxicity. Cytotoxicity was measured using the calcein release assay and the contribution of different death effector pathways was analyzed using specific inhibitors.
RESULTS: Treatment with IFNβ induced TRAIL expression on patients' NK cells and increased their cytotoxicity against NPC targets in vitro. NK cell-mediated cytotoxicity was predominately mediated via TRAIL. IFNβ also induced the production of soluble TRAIL (sTRAIL) by NK cells and its release upon contact with NPC cells. IFNβ treatment increased serum levels of sTRAIL in patients. Moreover, sTRAIL concentrated from patients' serum samples induced apoptosis ex vivo in NPC cells from a patient-derived xenograft.
CONCLUSION: Increased cytotoxicity of NK cells against NPC cells and increased serum levels of biologically active TRAIL in patients treated with IFNβ could be a means to eliminate micrometastatic disease and explain the low systemic relapse rate in this patient group.
Metabolic tumor volume and conformal radiotherapy based on prognostic PET/CT for treatment of nasopharyngeal carcinoma.
Medicine (Baltimore). 2019; 98(28):e16327 [PubMed] Free Access to Full Article Related Publications
Oncologic outcomes of IMRT versus CRT for nasopharyngeal carcinoma: A meta-analysis.
Medicine (Baltimore). 2019; 98(24):e15951 [PubMed] Free Access to Full Article Related Publications
METHODS: A literature search was performed through PubMed, Embase, and the Cochrane library databases from their inceptions to November 10, 2018. Two authors assessed the included studies and extracted data independently. Relative studies that compared oncologic outcomes between CRT and IMRT for NPC were included.
RESULTS: A total of 13 eligible studies were included, which contained 1 RCT, 1 prospective study, and 11 retrospective studies. Our meta-analysis showed that IMRT has increased overall survival (OR = 0.51, 95% CI = 0.41-0.65, P < .00001), locoregional control rate (OR = 0.59, 95% CI = 0.52-0.67, P < .00001), disease-free survival (OR = 0.77, 95% CI = 0.65-0.91, P = .002), and metastasis-free survival (OR = 0.71, 95% CI = 0.54-0.94, P = .01) in comparison with CRT.
CONCLUSION: The results of this meta-analysis indicate IMRT should be a better option for the treatment of NPC because patients who underwent IMRT may benefit from increased overall survival, locoregional control rate, disease-free survival, and metastasis-free survival compared with CRT.
Nasopharyngeal carcinoma.
Lancet. 2019; 394(10192):64-80 [PubMed] Related Publications
miR-205-5p regulates epithelial-mesenchymal transition by targeting PTEN via PI3K/AKT signaling pathway in cisplatin-resistant nasopharyngeal carcinoma cells.
Gene. 2019; 710:103-113 [PubMed] Related Publications
High/positive expression of ERCC1 predicts poor treatment response and survival prognosis in nasopharyngeal carcinoma: A systematic meta-analysis from 21 studies.
Medicine (Baltimore). 2019; 98(21):e15641 [PubMed] Free Access to Full Article Related Publications
OBJECTIVES: In an attempt to address this issue, we conducted the present comprehensive meta-analysis.
DATA SOURCES: Studies published until November 2017 were searched. Finally, total 21 literatures involving 22 cohorts and 2921 NPC patients fulfilled the inclusion criteria.
RESULTS: The pooled results showed that high/positive expression of ERCC1 predicted poor objective response rate (ORR) [odds ratio (OR) = 2.83; 95% confidence interval (CI) = 2.11-3.80; P <.001], overall survival (OS) [hazard ratio (HR) = 1.77; 95% CI = 1.48-2.12; P <.001], and disease-free survival (DFS) (HR = 1.60; 95% CI = 1.43-1.79; P <.001) in NPC. Low heterogeneity was detected among these studies (ORR: I = 0.0%, P = .776; DFS: I = 38.7%, P = .148; OS: I = 0.0%; P = .530). The results of sensitivity analyses and publication bias verified the reliability of our findings.
CONCLUSIONS: This study suggested ERCC1 as a potential predictive and prognostic biomarker for the treatment response and survival prognosis of NPC patients.
Accuracy of Raman spectroscopy in discrimination of nasopharyngeal carcinoma from normal samples: a systematic review and meta-analysis.
J Cancer Res Clin Oncol. 2019; 145(7):1811-1821 [PubMed] Related Publications
METHODS: We searched six databases (PubMed, Embase, Cochrane Library, Web of Science, Scopus and CNKI) up to September 2018 for all published studies that assessed the diagnostic accuracy of RS in the detection of nasopharyngeal carcinomas. Non-qualifying studies were screened out in accordance with the specified exclusion criteria and relevant information about the diagnostic performance of RS extracted. A random effects model was adopted to calculate the pooled sensitivity, specificity, positive and negative likelihood ratios (PLR and NLR, respectively), diagnostic threshold and diagnostic odds ratio (DOR). Additionally, we conducted a summary receiver-operating characteristic (SROC) curve analysis and threshold analysis, reporting area under the curve (AUC) to evaluate the overall performance of RS.
RESULTS: Three studies examined RS analysis in vivo, the pooled sensitivity and specificity of RS of which were 0.90 and 0.91, respectively, with an AUC of 0.9617. Eighteen studies assessed ex vivo samples, for which RS exhibited particularly high accuracy for the analysis of blood plasma.
CONCLUSIONS: RS was demonstrated to be a reliable technique for the detection of nasopharyngeal carcinoma with high accuracy, but additional studies are required to improve its performance and expand its application in ex vivo detection.
Circulating miR-31-5p may be a potential diagnostic biomarker in nasopharyngeal carcinoma.
Neoplasma. 2019; 2019 [PubMed] Related Publications
Induction chemotherapy plus IMRT alone versus induction chemotherapy plus IMRT-based concurrent chemoradiotherapy in locoregionally advanced nasopharyngeal carcinoma: a retrospective cohort study.
J Cancer Res Clin Oncol. 2019; 145(7):1857-1864 [PubMed] Related Publications
METHOD: We analyzed data from patients with locoregionally advanced NPC (stage III-IVb) who were treated at the West China hospital between January 2008 and December 2014. Patients received docetaxel, cisplatin, and 5-fluorouracil (TPF) IC followed by IMRT alone (IC + RT group) or IMRT plus cisplatin concurrent chemotherapy (IC + CCRT group). The main endpoint was overall survival (OS), which was evaluated by the Kaplan-Meier method and log-rank test. Multivariate Cox proportional hazard analysis was used to identify potential independent prognostic factors. Treatment-associated toxicities were compared between groups using the Chi squared test.
RESULTS: A total of 78 patients treated with IC + RT and 76 with IC + CCRT were analyzed. The median follow-up time was 59 months (range: 7-108 months). There was no difference between patients treated with IC + RT and IC + CCRT in terms of 3-year OS (89.0% versus 88.0%, p = 0.286), progression-free survival (76.8% versus 80.0%, p = 0.142), locoregional recurrence-free survival (87.1% versus 90.5%, p = 0.156), or distant metastasis-free survival (83.6% versus 82.6%, p = 0.567). Treatment (IC + RT versus IC + CCRT) was not an independent prognostic factor for OS (HR 1.425, 95% CI 0.698-2.908; p = 0.331). IC + CCRT was associated with a higher incidence of grade 3-4 neutropenia than IC + RT during radiotherapy (11.8% versus 1.3%, p = 0.020).
CONCLUSION: IC plus IMRT alone achieves similar patient survival outcomes as IC plus IMRT-based concurrent chemoradiotherapy, and has a lower incidence of toxicity.
Baicalein Exerts Anticancer Effect in Nasopharyngeal Carcinoma In Vitro and In Vivo.
Oncol Res. 2019; 27(5):601-611 [PubMed] Related Publications
Celastrol, a plant-derived triterpene, induces cisplatin-resistance nasopharyngeal carcinoma cancer cell apoptosis though ERK1/2 and p38 MAPK signaling pathway.
Phytomedicine. 2019; 58:152805 [PubMed] Related Publications
HYPOTHESIS/PURPOSE: The present study was designed to evaluate the cytotoxic effect and mode of action of a natural pentacyclic triterpenoid, celastrol, on cisplatin-resistant NPC cells.
RESULTS: Study results revealed that celastrol treatment significantly reduced the viability of NPC cells in dose and time dependent manners, as compared to untreated control cells. The cytotoxic effect of celastrol was mediated by cell cycle arrest at G2/M phase and induction of intrinsic and extrinsic apoptotic pathways. With further analysis, we observed that celastrol-induced activation of caspases was accompanied by increased phosphorylation of MAPK pathway proteins, p38, ERK1/2.
CONCLUSION: Taken together, our observation provides a novel insight on use of a natural plant product, celastrol, in the management of chemoresistant NPC.
Licochalcone A induces apoptotic cell death via JNK/p38 activation in human nasopharyngeal carcinoma cells.
Environ Toxicol. 2019; 34(7):853-860 [PubMed] Related Publications
MiR-1178-3p promotes the proliferation, migration and invasion of nasopharyngeal carcinoma Sune-1 cells by targeting STK4.
J Biol Regul Homeost Agents. 2019 Mar-Apr; 33(2):321-330 [PubMed] Related Publications
A unique case of eyelid metastasis from chondroid chordoma.
Indian J Pathol Microbiol. 2019 Apr-Jun; 62(2):287-289 [PubMed] Related Publications
Post-radiation sinusitis is associated with recurrence in nasopharyngeal carcinoma patients treated with intensity-modulated radiation therapy.
Radiat Oncol. 2019; 14(1):61 [PubMed] Free Access to Full Article Related Publications
METHODS: Two hundred and thirty patients with non-metastatic NPC were analyzed in terms of freedom from local failure (FFLF), freedom from distant failure (FFDF), overall survival (OS), and disease-free survival (DFS). For each patient, the status of the sinus mucosa was flexibly assessed by documenting mucosal changes as indicated by differences between images obtained before radiotherapy and more than 6 months post-radiation.
RESULTS: With a median follow-up of 39.7 months (8 to 81 months), 19 (8.26%) patients relapsed locally, 13 (5.65%) patients failed in the neck, and 26 (11.3%) patients developed distant metastases. The presence of sinusitis noted in images post-radiation was a significant predictor for DFS (p = 0.001), FFLF (p = 0.004), and FFDF (p = 0.015), in addition to having high negative predictive value for local relapse (97.5%).
CONCLUSIONS: This is the first study to investigate the prognostic value of post-radiation sinusitis in NPC patients treated with IMRT. Post-radiation sinusitis was found to be a significant predictor for DFS, FFLF, and FFDF, and was also found to have high negative predictive value for local recurrence (97.5%). It may thus be used as an additional tool for clinicians to determine the possibility of recurrence.
Prognostic value of the Epstein-Barr virus and tumor suppressor gene p53 gene in nasopharyngeal squamous cell carcinoma.
J Cancer Res Ther. 2019; 15(2):426-436 [PubMed] Related Publications
Results: The positive rate of EBERs hybridization and TP53 expressions was 76.3% and 52.2%, respectively, while the mutation rate of TP53 gene was 39.6%. Logistic regression analysis showed direct relationships between the subtypes of nasopharyngeal squamous cell carcinoma (NPSCC) and EBERs-positive, or frequent consumption of pickled food. Overall survival rates of patients with positive TP53 expression, the TP53 gene mutations, vascular invasions, organ metastases, lymph node metastasis, and clinical recurrence were significantly lower than those of patients without those symptoms. The poorer prognosis was related to regularly drinking and the advanced age. According to the Cox regression analysis, we found that the main prognostic factors of NPSCC patients were the aging, recurrence, TP53 gene mutations, especially exon 7 or 8 mutations.
Conclusions: We concluded that there were the correlations between NPSCC subtypes with EBV infection and frequent intaking of pickled food, while aging, clinical recurrence, and TP53 gene mutations were independent predictors for the poor prognosis of nasopharyngeal carcinoma.
Nasopharyngeal cancer combination chemoradiation therapy based on folic acid modified, gefitinib and yttrium 90 co-loaded, core-shell structured lipid-polymer hybrid nanoparticles.
Biomed Pharmacother. 2019; 114:108820 [PubMed] Related Publications
PGC1α/CEBPB/CPT1A axis promotes radiation resistance of nasopharyngeal carcinoma through activating fatty acid oxidation.
Cancer Sci. 2019; 110(6):2050-2062 [PubMed] Free Access to Full Article Related Publications
Bioinformatic identification of candidate biomarkers and related transcription factors in nasopharyngeal carcinoma.
World J Surg Oncol. 2019; 17(1):60 [PubMed] Free Access to Full Article Related Publications
METHODS: We investigated two microarray profile datasets GSE64634 and GSE12452 to screen the potential differentially expressed genes (DEGs) in NPC. Gene ontology and Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment analysis of the DEGs were also performed. A protein-protein interaction (PPI) network of DEGs was constructed by STRING and visualized by Cytoscape software. The associated transcriptional factor regulatory network of the DEGs was also constructed.
RESULTS: A total of 152 DEGs were identified from the GSE64634 and GSE12452 datasets, including 10 upregulated and 142 downregulated genes. Gene functional enrichment analysis indicated that these DEGs were enriched in the cilium movement, antimicrobial humoral response, O-glycan processing, mucosal immune response, carbohydrate transmembrane transporter activity, hormone biosynthetic process, neurotransmitter biosynthetic process, and drug metabolism-cytochrome P450 pathway. Five hub genes (DNALI1, RSPH4A, RSPH9, DNAI2, and ALDH3A1) and one significant module (score = 5.6) were obtained from the PPI network. Key transcriptional factors, such as SPI1, SIN3B, and GATA2, were identified with close interactions with these five hub DEGs from the gene-transcriptional factor network.
CONCLUSIONS: With the integrated bioinformatic analysis, numerous DEGs related to NPC were screened, and the hub DEGs we identified may be potential biomarkers for NPC.
Pretreatment MRI radiomics analysis allows for reliable prediction of local recurrence in non-metastatic T4 nasopharyngeal carcinoma.
EBioMedicine. 2019; 42:270-280 [PubMed] Free Access to Full Article Related Publications
METHODS: A total of 737 patients from Sun Yat-sen University Cancer Center (training cohort: n = 360; internal validation cohort: n = 120) and Wuzhou Red Cross Hospital (external validation cohort: n = 257) underwent feature extraction from the largest axial area of the tumor on pretreatment magnetic resonance imaging scans. Feature selection was based on the prognostic performance and feature stability in the training cohort. Radscores were generated using the Cox proportional hazards regression model with the selected features in the training cohort and then validated in the internal and external validation cohorts. We also constructed a nomogram for predicting local recurrence-free survival (LRFS).
FINDINGS: Eleven features were selected to construct the Radscore, which was significantly associated with LRFS. For the training, internal validation, and external validation cohorts, the Radscore (C-index: 0.741 vs. 0.753 vs. 0.730) outperformed clinical prognostic variables (C-index for primary gross tumor volume: 0.665 vs. 0.672 vs. 0.577; C-index for age: 0.571 vs. 0.629 vs. 0.605) in predicting LRFS. The generated radiomics nomogram, which integrated the Radscore and clinical variables, exhibited a satisfactory prediction performance (C-index: 0.810 vs. 0.807 vs. 0.753). The nomogram-defined high-risk group had a shorter LRFS than did the low-risk group (5-year LRFS: 73.6% vs. 95.3%, P < .001; 79.6% vs 95.8%, P = .006; 85.7% vs 96.7%, P = .005).
INTERPRETATION: The Radscore can reliably predict LRFS in patients with non-metastatic T4 NPC, which might guide individual treatment decisions. FUND: This study was funded by the Health & Medical Collaborative Innovation Project of Guangzhou City, China.
The diagnostic and prognostic values of plasma Epstein-Barr virus DNA for residual cervical lymphadenopathy in nasopharyngeal carcinoma patients: a retrospective study.
Cancer Commun (Lond). 2019; 39(1):14 [PubMed] Free Access to Full Article Related Publications
METHODS: This study included 82 NPC patients who were diagnosed with suspected residual cervical lymphadenopathy following completion of antitumor therapy. Their plasma EBV DNA levels were measured using quantitative polymerase chain reaction (qPCR) before the initiation of treatment and before neck dissection. Fine needle aspiration cytology (FNAC) was performed in 21 patients. All patients had undergone neck dissection and postoperative pathological examination to identify the nature of residual cervical lymphadenopathy. The overall survival (OS), progression-free survival (PFS), distant metastasis-free survival (DMFS), and locoregional relapse-free survival (LRRFS) were calculated using the Kaplan-Meier method and compared using the log-rank test. The Cox proportional hazards model was used to calculate hazard ratios (HRs) with 95% confidence intervals (CIs). Multivariable analysis was used to estimate the effect of potential prognostic factors on survival.
RESULTS: Following a median follow-up of 52.6 months, compared with patients with negative postoperative pathological findings for residual cervical lymphadenopathy, the patients with positive findings had a significantly lower 3-year PFS rate (49.9% vs. 83.3%, P = 0.008). Among NPC patients with residual cervical lymphadenopathy, the patients with preoperative plasma EBV DNA > 0 copy/mL had a lower 3-year PFS rate than did those with no detectable EBV DNA (43.7% vs. 61.1%, P = 0.031). In addition, combining FNAC with preoperative EBV DNA detection improved the diagnostic sensitivity. Multivariable analysis demonstrated that residual cervical lymphadenopathy with positive postoperative pathological result was an independent prognostic factor for PFS and that detectable preoperative plasma EBV DNA was an independent prognostic factor for OS.
CONCLUSIONS: Using FNAC combined with preoperative EBV DNA detection improves the sensitivity in diagnosing NPC with residual cervical lymphadenopathy. Compared with patients with undetectable EBV DNA, patients with detectable preoperative plasma EBV DNA have worse prognosis and may require a more aggressive treatment strategy.
Expression of LEF1 and TCF1 (TCF7) proteins associates with clinical progression of nasopharyngeal carcinoma.
J Clin Pathol. 2019; 72(6):425-430 [PubMed] Related Publications
METHODS: We collected 391 cases of NPC, 53 non-cancerous control nasopharyngeal mucosa and 28 pairs of NPC and their matched metastases, detected expression of LEF1 and TCF1 (TCF7) proteins in these tissues by immunohistochemistry. RESULTS: Results showed that there were significantly increased expression of both LEF1 and TCF1 (TCF7) proteins and coexpression of LEF1 and TCF1 (TCF7) in NPC than these in non-cancerous nasopharyngeal mucosa (all p<0.001), as well as LEF1 and coexpression of LEF1 and TCF1 (TCF7) in matched metastasis NPCs than these in the primary NPCs (p=0.003 and p=0.014, respectively). In addition, expression of LEF1 and the coexpression of LEF1 and TCF1 (TCF7) proteins were positively correlated with lymph node metastasis (p=0.001 and p=0.020, respectively), advanced clinical stage (p<0.003 and p=0.027, respectively) and poor survival status of patients with NPC (p<0.001 and p=0.004, respectively). Moreover, multivariate Cox regression analysis identified that the positive expression of LEF1 was the independent poor prognostic factor for overall survival of patients with NPC (p<0.001).
CONCLUSIONS: The expression of LEF1 associated positively with TCF1 (TCF7) and clinical progression of NPC, and positive expression of LEF1 protein may act as valuable independent biomarker to predict poor prognosis for patients with NPC.
Ginsenoside Rg3 Inhibits Migration and Invasion of Nasopharyngeal Carcinoma Cells and Suppresses Epithelial Mesenchymal Transition.
Biomed Res Int. 2019; 2019:8407683 [PubMed] Free Access to Full Article Related Publications
Application of a machine learning method to whole brain white matter injury after radiotherapy for nasopharyngeal carcinoma.
Cancer Imaging. 2019; 19(1):19 [PubMed] Free Access to Full Article Related Publications
METHODS: A DTI scan was performed in 77 patients and 67 normal controls. A fractional anisotropy map was generated by DTIFit. TBSS was used to find the region where the FA differed between the case and control groups. Each resulting FA value image is registered with each other to create an average FA value skeleton. Each resultant FA skeleton image was connected to feature vectors, and features with significant differences were extracted and classified using a support vector machine (SVM). Next, brain segmentation was performed on each subject's DTI image using automated anatomical labeling (AAL), and deterministic white matter fiber bundle tracking was performed to generate symmetrical brain matrix, select the upper triangular component as a classification feature. Two-sample t-test was used to extract the features with significant differences, then classified by SVM. Finally, we adopted a permutation test and ROC curves to evaluate the reliability of the classifier.
RESULTS: For FA, the accuracy of classification between the 0-6, 6-12 and > 12 months post-RT groups and the control group was 84.5, 83.9 and 74.5%, respectively. In the case groups, the FA with discriminative ability was reduced, mainly in the bilateral cerebellum and bilateral temporal lobe, with prolonged time, the damage was aggravated. For WM connections, the SVM classifier classification recognition rates of the 0-6, 6-12 and > 12 months post-RT groups reached 82.5, 78.4 and 76.3%, respectively. The WM connections with discriminative ability were reduced.
CONCLUSIONS: RBI is a disease involving whole brain WM network anomalies. These brain discriminating WM regions and WM connection modes can supplement the understanding of RBI and be used as biomarkers for the early clinical diagnosis of RBI.
Short-term stimulation with histone deacetylase inhibitor trichostatin a induces epithelial-mesenchymal transition in nasopharyngeal carcinoma cells without increasing cell invasion ability.
BMC Cancer. 2019; 19(1):262 [PubMed] Free Access to Full Article Related Publications
METHODS: Poorly-differentiated NPC cell line CNE2 and undifferentiated C666-1 were treated with various concentrations of TSA, the cell viability was assessed by CCK-8 assay, the morphology was photographed, and the mRNA level of HDACs was assessed by semiquantitative PCR. After determination the cell cycle distributions, cells were subjected to western blotting analysis of cell cycle and EMT-associated genes expression. And the changes in migration ability were assessed by transwell migration assay and scratch wound healing assay. Finally, histone deacetylases activator ITSA-1 was used to assess the reverse of TSA-induced changes in NPC cells.
RESULTS: TSA inhibited the proliferation of CNE2 and C666-1 cells in a concentration-dependent manner and arrested the cell cycle at G1 phases. TSA reduced PCNA, cyclin D1, cyclin E1, CDK2, p16 and p21 expressions and stimulated CDK6 levels. TSA stimulation for 48 h could effectively induce the EMT in CNE2 and C666-1 cells, which showed an increase of spindle-like cells and promoted expression of Vimentin and Snail1 expression in a concentration-dependent manner. Surprisingly, this short period of TSA treatment that induced EMT also impeded the migration ability of CNE2 and C666-1 cells. Interestingly, ITSA-1 rescued TSA-impeded CNE2 and C666-1 cells' proliferation, migration and HDACs expression, also re-induced the cells to turn into epithelial cell phenotypes.
CONCLUSIONS: These results indicate that short-term stimulation of TSA effectively inhibits cell proliferation and induce EMT-like changes in NPC cells but not increase its invasion ability.
The Long Noncoding RNA NEAT1 Targets miR-34a-5p and Drives Nasopharyngeal Carcinoma Progression via Wnt/β-Catenin Signaling.
Yonsei Med J. 2019; 60(4):336-345 [PubMed] Free Access to Full Article Related Publications
MATERIALS AND METHODS: Quantitative real-time PCR assay was performed to assess the expression of NEAT1 and miR-34a-5p in NPC tissues and cells. Western blot analysis was used to observe cell epithelial to mesenchymal transition (EMT) and the activation of Wnt/β-catenin signaling in 5-8F cells. MiRNA directly interacting with NEAT1 were verified by dual-luciferase reporter assay and RNA immunoprecipitation. Cell proliferation ability was determined by CCK-8 assay, and cell migration and invasion capacities were assessed by transwell assays. An animal model was used to investigate the regulatory effect of NEAT1 on tumor growth
RESULTS: Our data revealed that NEAT1 is upregulated, while miR-34a-5p is downregulated in NPC tissues and cell lines. NEAT1 knockdown repressed tumor growth
CONCLUSION: Our study demonstrated that NEAT1 targets miR-34a-5p at least partly to drive NPC progression by regulating Wnt/β-catenin signaling, suggesting a potential therapeutic target for NPC.
Long non-coding RNA 520 is a negative prognostic biomarker and exhibits pro-oncogenic function in nasopharyngeal carcinoma carcinogenesis through regulation of miR-26b-3p/USP39 axis.
Gene. 2019; 707:44-52 [PubMed] Related Publications
Keratin 6A gene silencing suppresses cell invasion and metastasis of nasopharyngeal carcinoma via the β‑catenin cascade.
Mol Med Rep. 2019; 19(5):3477-3484 [PubMed] Free Access to Full Article Related Publications

 MTOR
MTOR